Brief Facts: Septal Perforation Overview
This document briefly discusses the pathophysiology of a perforated septum and the benefits of early septal perforation repair.
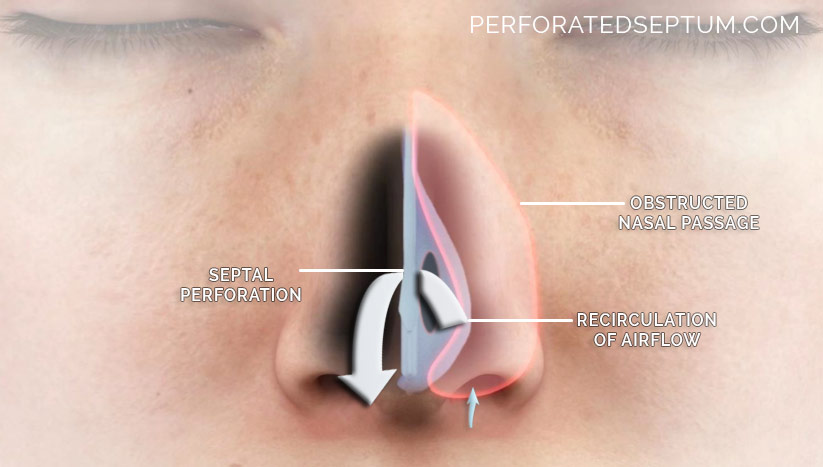
Definition: Septal perforation is a hole in the nasal septum, caused by an injury.
Symptoms: Whistling, nosebleeds, foul smelling crust, recurrent infections, nasal congestion, sinusitis, and nasal collapse deformity are the most common symptoms associated with septal perforation.
Treatment: Treatment options vary based on the size of the septal perforation. Generally all perforations, regardless of their size, should be treated aggressively to prevent complications. Medical, minimally invasive, and surgical options are selected based on the size of the perforation at initial diagnosis. Dr. Hamilton’s preference is to intervene before symptoms lead to complications.
Recommendations: Currently we recommend permanently repairing all septal perforations and have had a 100% success rate in improving symptoms.
Video: Frequently Asked Septal Perforation Questions
Dr. Hamilton answers frequently asked questions about septal perforation and treatment options.
Video: Perforated Septum Repair
for Patient with Hereditary Bleeding Disorder-HHT
HHT is a hereditary condition that causes fragile malformed blood vessels. After many trips to the emergency room to cauterize and stop nose bleeds, David is left with a large hole in his septum that must be fixed.
What is a Perforated Septum?
A septal perforation is a through-and-through hole in the central partition of the nose (nasal septum).
The septum is the central partition in the nose, which is made up of wafer thin cartilage and bone protected by a delicate mucosal membrane. Septal perforations occur most commonly from an insult to this delicate septal mucosa, which supplies blood, oxygen, and vital nutrients to the underlying cartilage, which has no blood supply of its own. The most common injuries are trauma, surgery, and medication or illicit drug abuse. A septal perforation is a through-and-through hole in the central partition of the nose (nasal septum). What does a septal perforation look like? The septum is responsible for maintaining laminar airflow through the nose. A perforated septum causes abnormal airflow in the nasal passages. This leads to over drying, crusting, infection, and if untreated, enlargement of the perforation which intensifies the symptoms.
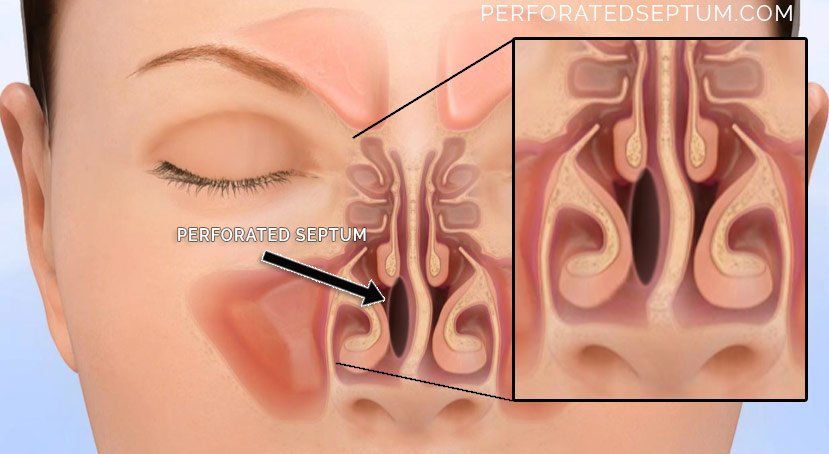
How Does A Perforated septum Affect My Breathing?
The physiology of airflow through the nose is not complicated. Inspired air flows uniformly over the nasal turbinates, which add heat and moisture to the air. By the time the air reaches our lungs it is warmed and humidified supporting comfortable breathing. The nose is nature’s humidifier. When we are congested (such as with a cold) and we breathe through our mouth at night we awake with a sore dry throat. The nose is not necessary for breathing, just to do so comfortably.
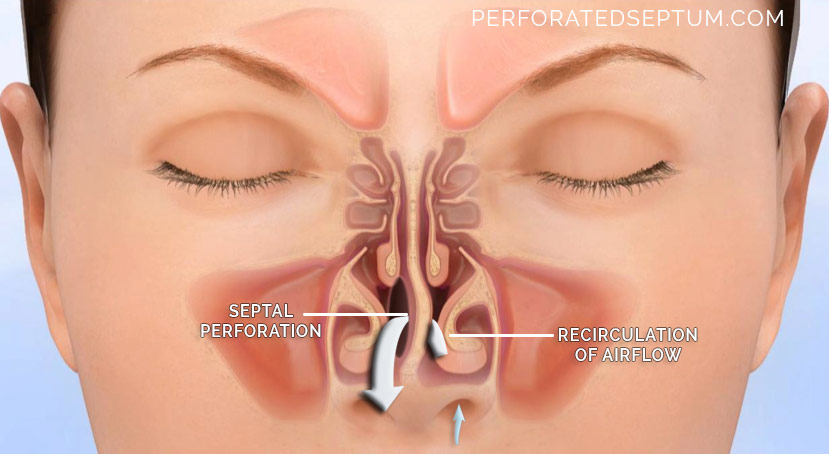
When the septum is perforated the normal pattern of airflow through the nose is disrupted. Inspired air beings to recirculate, swirling through the nose, much like calm flowing water turning to rapids in a stream. The recirculation of inspired air “steals” more than its fair share of moisture and heat on its way back out of the nose through the perforation causing excessive drying of the delicate nasal mucosa. Alternately inspired air may simply become trapped in the perforation like a whirlpool. This abnormal airflow through the nose leads to excessive drying of the mucosal membrane. The septal perforation itself becomes crusted, bloody, and occasionally infected with bacteria that easily penetrate the damaged mucosa and cartilage.
Patients often present to their physician with blocked nasal passages from excessive crusts, foul smelling pus in the nose, and nosebleeds. If the septal perforation is left untreated the crust, infection, and bleeding damage more cartilage and the septal perforation slowly becomes larger destabilizing the nose leading to potential collapse and worsening symptoms.
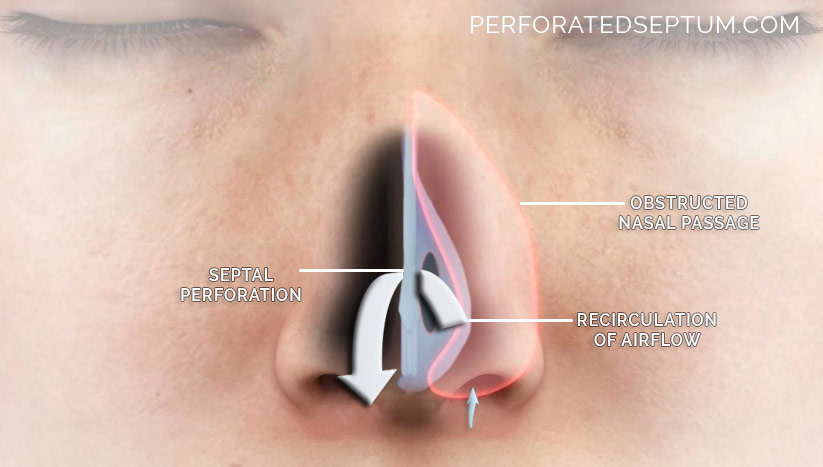
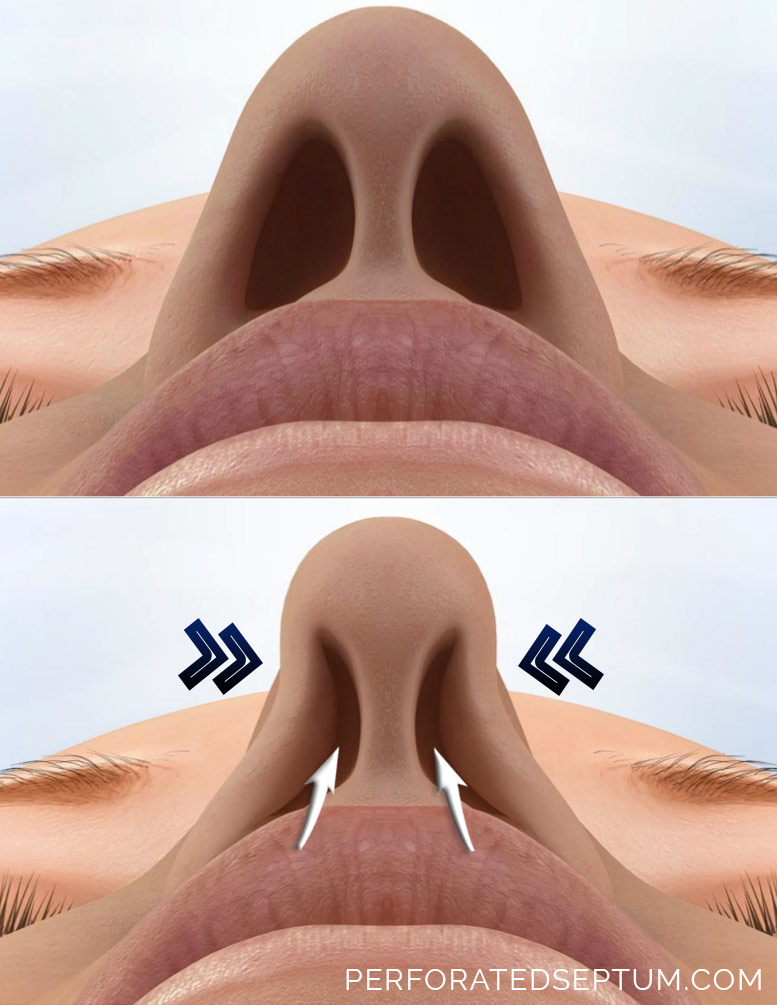
Septal perforation causes recirculation of inspired air. This illustration demonstrates air flowing through the left nasal passage (yellow arrow). The white arrow represents nasal airflow recirculation through the septal perforation (dotted arrow) into the right nasal passage from the left nasal passage. The swirling air is like a small tornado inside the nose reeking havoc on the nasal septum causing the hole (septal perforation) to enlarge overtime.
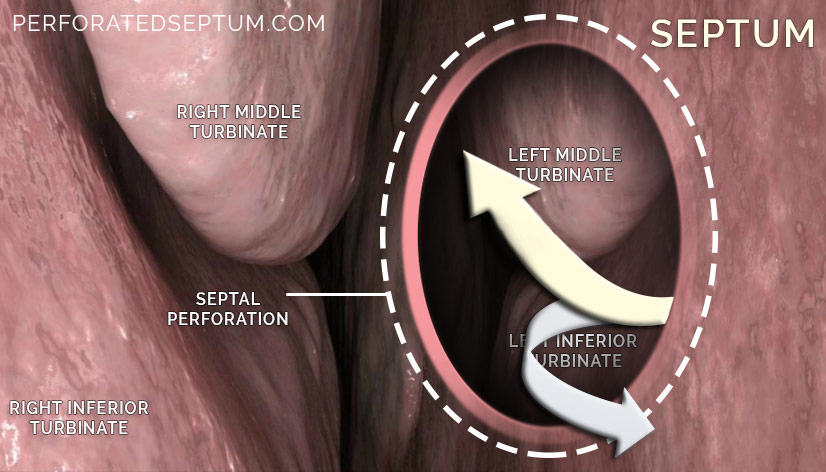
SEPTAL PERFORATION ANATOMY
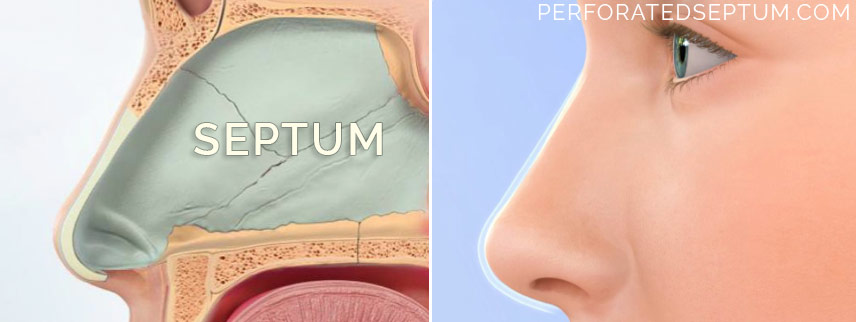
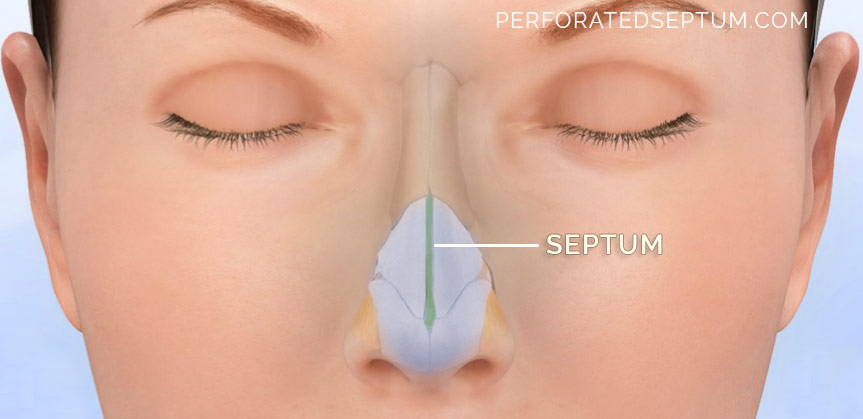
What is the nasal septum?
The nasal septum divides the nose into right and left nasal passages and is made up of delicate skin, mucosa, cartilage and paper thin bones that provide the central support and foundation for the nose. Functionally, the normal septum insures that air flowing through the nose is moving through the nasal passages gently in a laminar fashion without turbulence and is evenly distributed between the nasal passages. This is important because functionally speaking your nose is simply a compact humidifier for the air that you breathe.
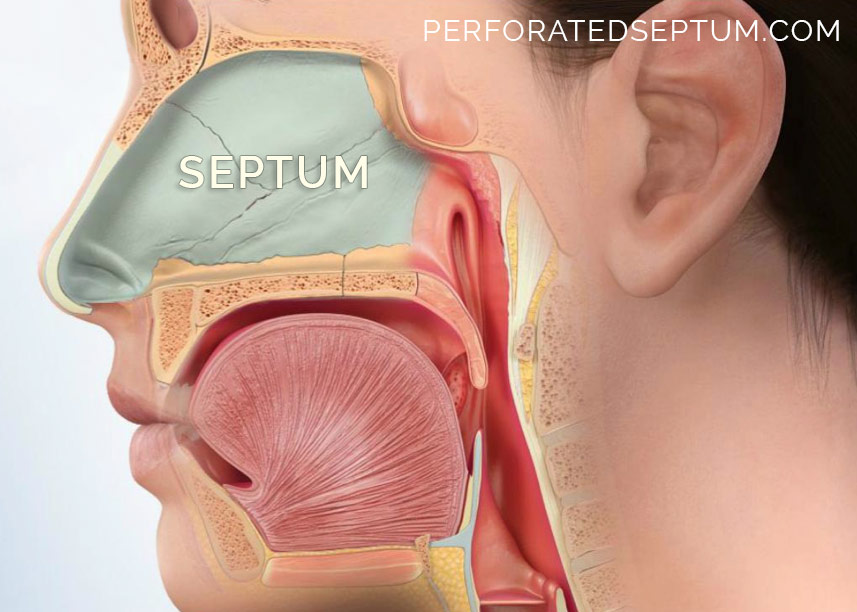
The nasal septum divides the nose into two separate humification chambers. Each side of the nose shares the workload of conditioning the air we breathe. The nasal turbinates swell slightly ever 4-6 hours diverting more airflow form side to side allowing each chambers to rest throughout the day.
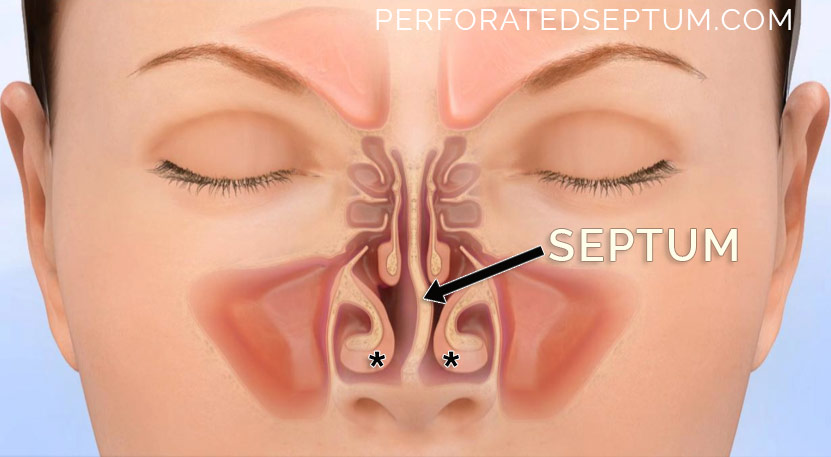
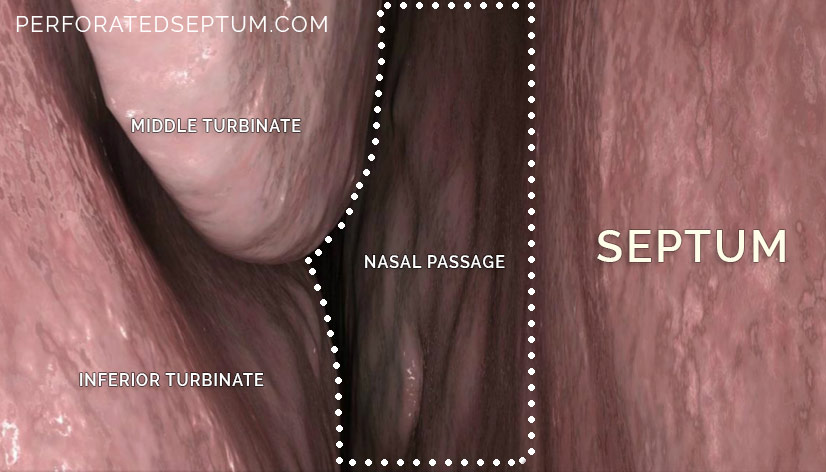
SEPTAL PERFORATION CAUSES & SYMPTOMS
WHAT ARE THE COMMON CAUSES OF a Perforated septum?
Septal perforations are caused by an injury to the nasal septum. The septum is very delicate and can be easily injured by trauma (nasal fracture), infection (MRSA), medication or drug abuse (nasal decongestants, nasal steroids, or cocaine), autoimmune conditions, and by prior surgery such as septoplasty or rhinoplasty. A hole in the septum is diagnosed as a septal perforation, or perforated septum.
Causes for Septal Perforation:
- Trauma
- Septal Hematoma
- Infection
- Medication Nasal Spray Overuse
- Drug Abuse
- Autoimmune Disorders (Wegerner’s Granulomatosis)
- Septoplasty
- Rhinoplasty
WHAT ARE THE SYMPTOMS OF SEPTAL PERFORATION?
Septal perforation symptoms include nosebleeds, foul odors, crusting, infection, nasal deformity and instability.
Untreated septal perforations typically enlarge over time and become more symptomatic effecting the normal functions and structure of the nose. Symptoms range in type and severity depending on the location and size of the perforation from whistling, foul smelling nasal discharge, nasal crusting, nose bleeds, obstructed nasal breathing, snoring, increase susceptibility to infections, and nasal collapse and cosmetic deformity. The severity of symptoms can vary from mild to severely debilitating. Typically patients may also have other nasal conditions that further exacerbate their symptoms such as nasal obstruction from failed rhinoplasty, a deviated septum, enlarged turbinates, sinus disease, and allergy.
Symptoms of a perforation include:
- Whistling from the nose while breathing
- Nosebleeds
- Foul-smelling crust
- Recurrent infections
- Nasal congestion
- Sinusitis
- Nasal obstruction
SEPTAL PERFORATION DIAGNOSIS
HOW IS A PERFORATED SEPTUM DIAGNOSED?
A septal perforation can be diagnosed on routine nasal exam or nasal endoscopy. More importantly however is determining the cause of the septal perforation. The etiology of a septal perforation is paramount in effective treatment planning by Dr. Hamilton. We must know the cause of the septal perforation to prevent further recurrence after treatment. This is especially true for patients with undiagnosed autoimmune disorders such Wegerner’s granulomatosis which causes systemic effects outside the nose and needs to be treated concomitantly or patients with behavioral habits (i.e. compulsive nose picking) that will need to be addressed before septal perforation treatment.
Unfortunately, many patients presenting to the doctor are initially unaware that they have a septal perforation. These patients may simply have sought evaluation by their primary care physician or local ENT (Ear, Nose, & Throat doctor) for a more benign condition such as a recurrent nosebleed, sinus congestion, or nasal pain, only to be told that they have a septal perforation, which is often a shock. Other patients have self-diagnosed themselves as septal perforation patients and may have chronic habits that have caused the perforation (i.e. nose picking). More shocking than the diagnosis is that many patients are falsely told that there is nothing that can be done outside of ointments and a septal button. Most patients amount these treatments to doing nothing. Patients seek out Dr. Hamilton for more treatment options.
Diagnosis begins with a routine history and physical examination.
Nasal Exam
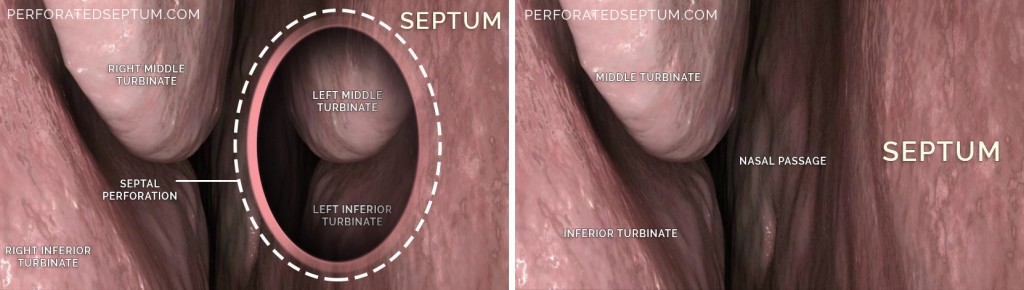
The nasal septum is examined with a nasal speculum and a headlight or mirror. The intact septum is healthy and pink and is free of crusting, bloody, and fetid secretions. The patient may have a deviated septum (as below) but this is a normal variant in many nasal exams and does not equal the diagnosis of a septal perforation.
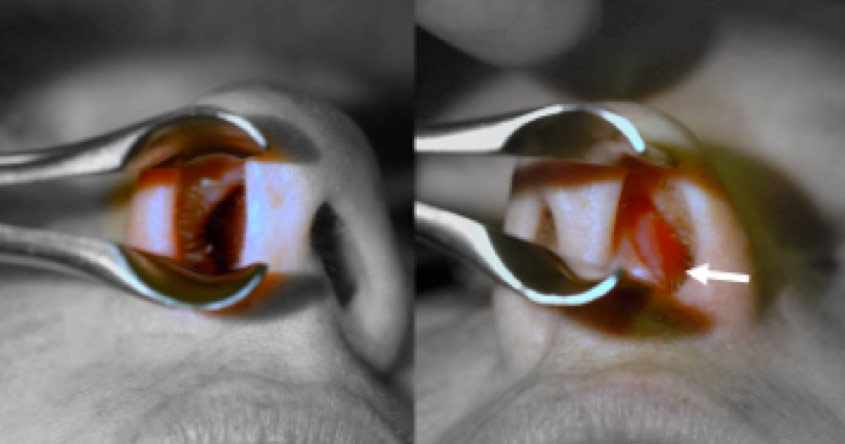
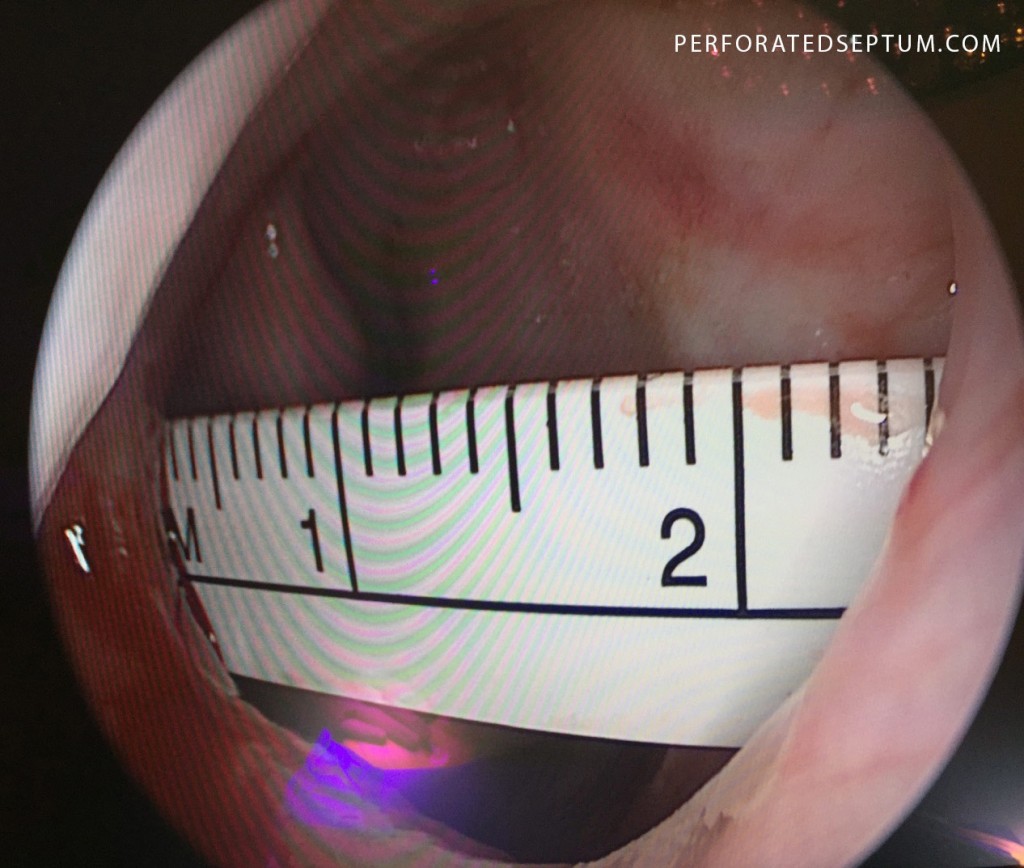
Nasal Endoscopy
A more thorough nasal examination can be performed with a nasal endoscope. This telescopic lens magnifies and illuminates the nasal cavity for a more complete examination of the internal nasal architecture. Nasal endoscopy can be used to accurately measure the size of the septal perforation, record video for surgical planning and diagnose any concomitant nasal disease such as a deviated septum, nasal polyps, sinus disease, or infections that may need treatment.
SEPTAL PERFORATION COMPLICATIONS
WHAT COMPLICATIONS ARE ASSOCIATED WITH a PERFORATED SEPTUM?
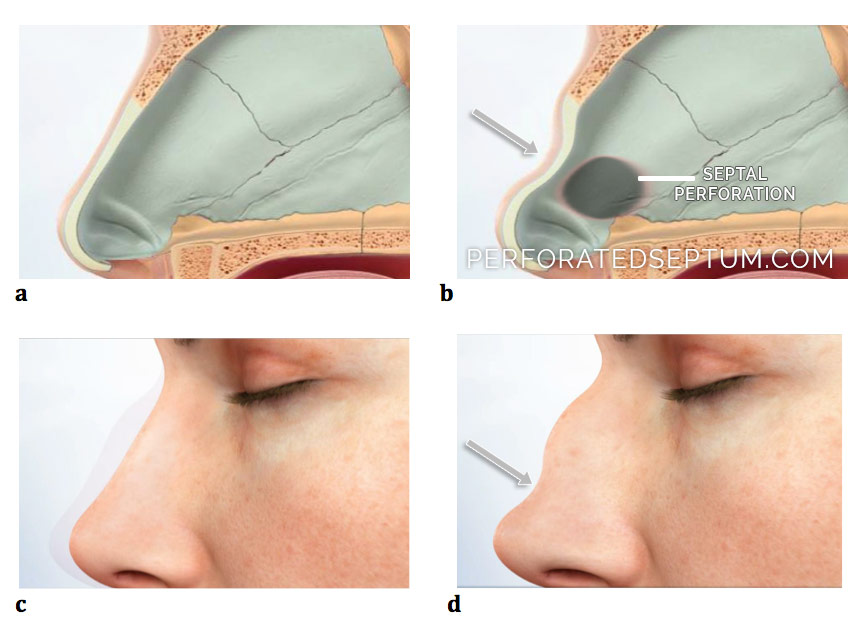
The nasal septum is the central support for the nasal skeleton. It is the foundation of a normal strong profile. The illustrations below represents the septum in profile supporting the overlying nasal structure. The overall nasal profile mirrors that of the septum profile. The nasal septum functionally stabilizes the nose much like a foundation supports and stabilizes a home or a skyscraper. Without a strong foundation a building will collapse. The nose is no different.
Septal perforations can destabilize the nose and lead to nasal collapse. This collapse most commonly occurs in the middle nasal region (cartilage at the middle of the nose called the middle vault) leading to structural weakening in that region. The middle nasal vault is destabilized and the nose collapses leaving a fixed saddle nose deformity. In rare cases patients who have a septal perforation and chronic infection (MRSA bacterial infections) may have collapse of the entire nasal cartilaginous framework (not just the septum) of the nose leading to collapse and deformity and twisting of the nose.
After the nose is further weakened by loss of its cartilage framework the entire nose may collapse dynamically with each inspiration. This is referred to as nasal valve collapse. This complication is seen most commonly in septal perforations associated with heavy cocaine abuse, but may also be seen in perforated noses caused by rhinoplasty. Learn more
Complications Include:
- Nasal Obstruction
- Saddle Nose Deformity
- Nasal Valve Collapse
- Cellulitis
- Turbinate Hypertrophy
- Chronic Nasal Pain
SEPTAL PERFORATION AND SADDLE NOSE DEFORMITY / NASAL DEFORMITY
Large septal perforations may cause structural compromise of the nose (deviation of the septum, saddle nose deformity, or collapse). Functional rhinoplasty, a structural surgery, focuses on re-establishing a natural aesthetic to the nose. The goal is to correct and prevent further collapse of the nasal skeleton and make the nose look normal. The structural rhinoplasty is best performed at the same time as the septal perforation repair. Learn more
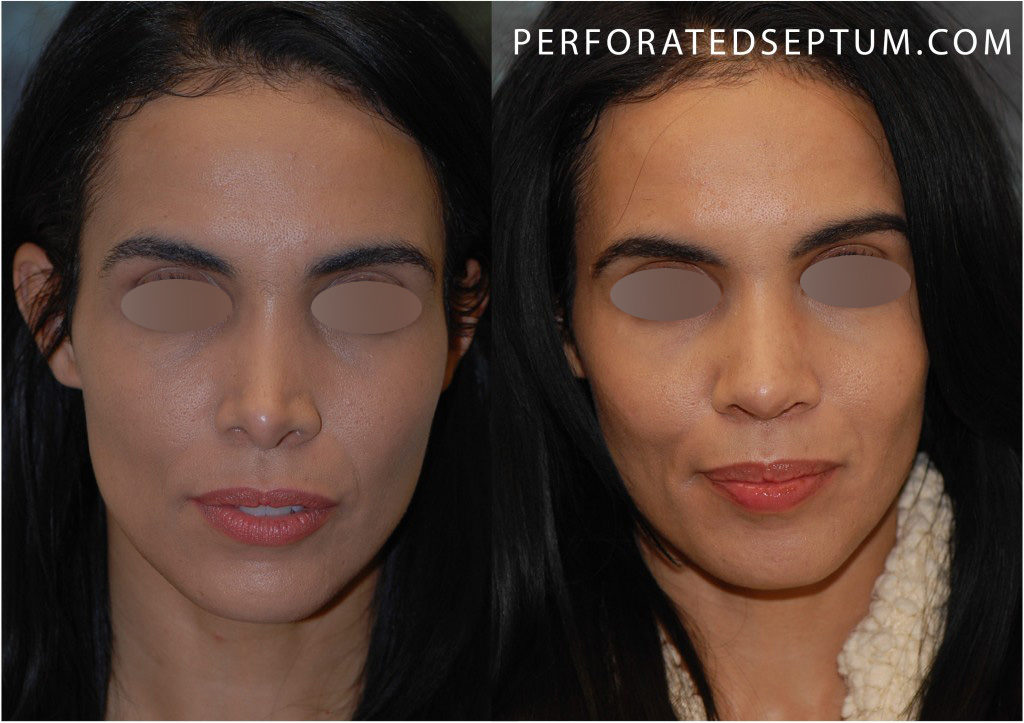


Nasal Deformity after cocaine abuse, Infection, & a pERFORATED SEPTUM
Snorting or “sniffing” cocaine through the nose may lead to a septal perforation. It is a fearful complication for those who have used cocaine. Cocaine works by constriction and eventually damages the delicate blood vessels that supply oxygen to the nasal septum mucosa. Without oxygen, the septal mucosal lining begins to necrosis (die). All the blood supply, nutrients and oxygen for the nasal septal cartilage comes form the overlying mucosa. Once the mucosa is irreversible damaged, it can no longer supply the cartilage beneath and the cartilage perforates. The perforated septum is unstable and the nose can collapse because of the weakened structural support of. Once present a septal perforation will not heal on its own. Learn more
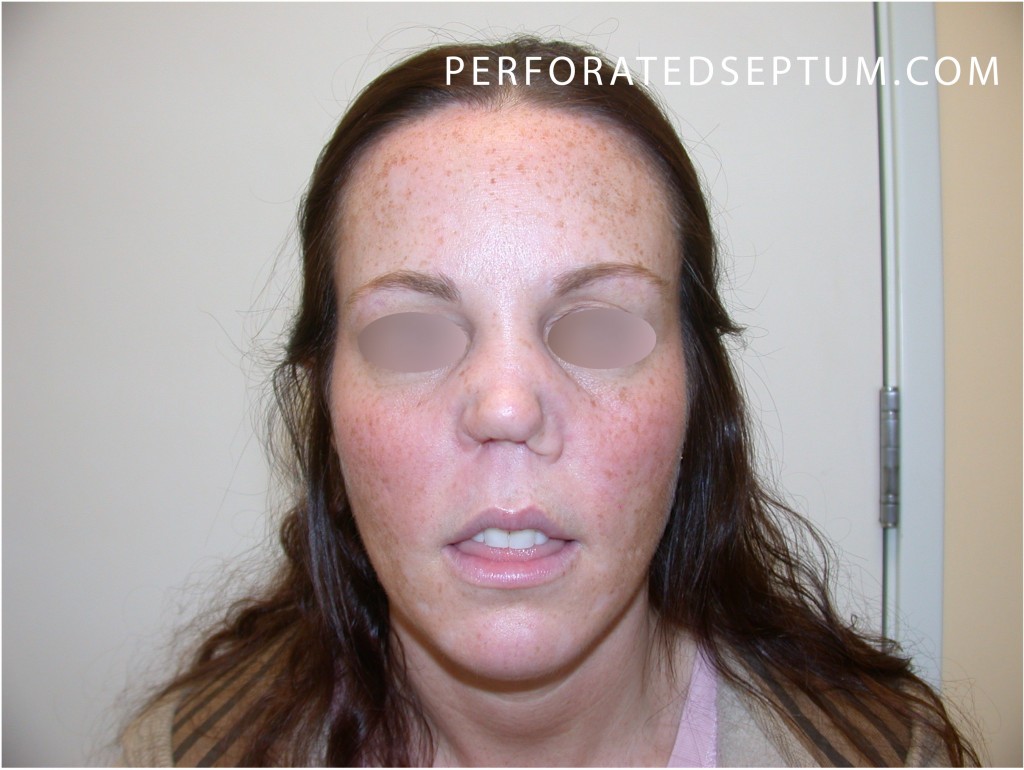
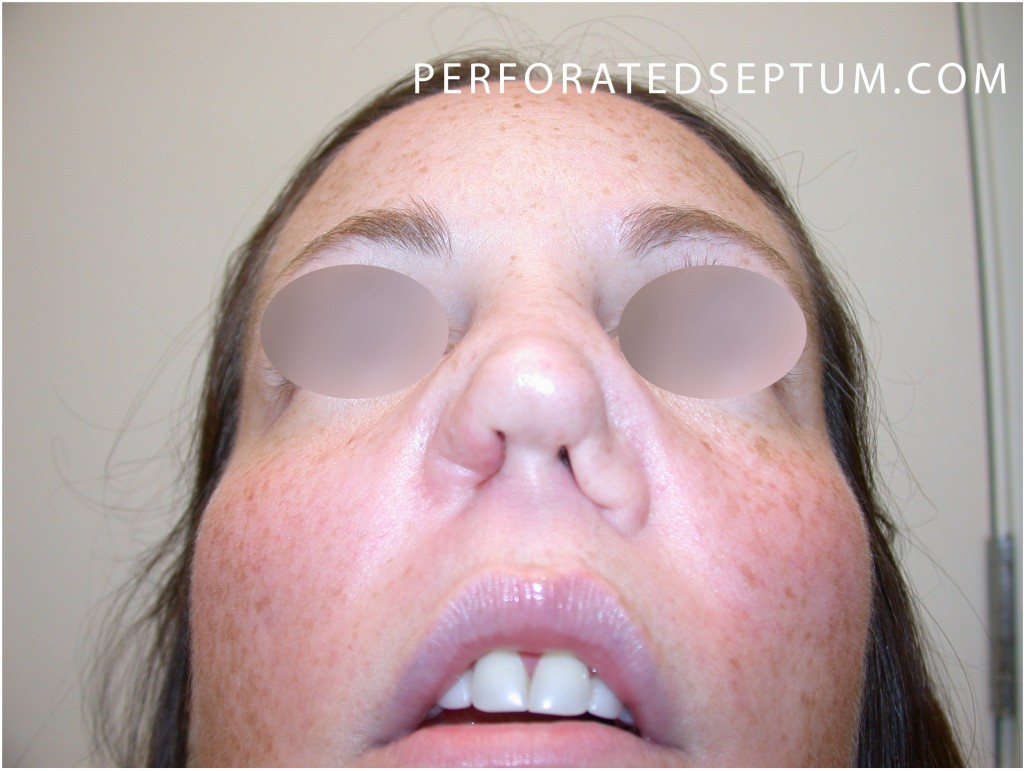
Septal Perforation Treatment
PERFORATED SEPTUM SURGERY AND REPAIR
Dr. Hamilton has designed several treatment regiments for patients based on size, symptoms, and individual patient goals. Comprehensively Dr. Hamilton’s goal to is make the patient symptom free and restore the nose functionally and structurally to its normal state and appearance. Treatment regiments typically included some or all of the following: a nasal disinfectant cleansing and debridement, increased humidification and moisture, correction or control of other concomitant nasal conditions, prevention of increase in the size of the perforation, surgical closure of the septal perforation, reconstruction of the normal nasal architecture.
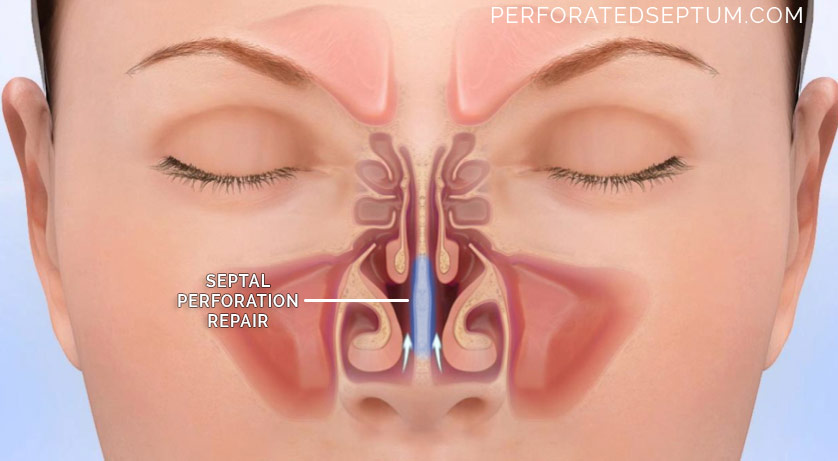
ALTERNATIVE TREATMENTS
All perforations should be treated to prevent long-term complications. The algorithmic management of a septal perforation is guided by the size of the perforation and severity of symptoms. Smaller perforations (<1cm) can be managed initially with humidification, antibiotic ointments and irrigation. Septal perforations 1-2cm in size should be initially managed with a septal button implant if symptoms are severe. The septal bottom covers the perforation and allows the lining around the perforation to heal.
In many institutions the septal button is left in permanently if the patient is comfortable and can tolerate the implant. If the patient cannot tolerate the implant, it can be used temporarily to stabilize the nose, prior to a permanent surgical repair. Septal perforations over > 2cm need to be repaired surgically and are not good candidates for septal buttons. Regardless the size of the perforation, Dr. Hamilton, believes that septal buttons should only be used as a temporary measure. In Dr. Hamilton’s experience most patients do not tolerate septal buttons indefinitely. Mucus accumulation around the septal button, implant rotation and uncontrolled pistoning of the implant inside the nose often leads to chronic irritation causing patients to request a permanent surgical option.
Dr. Hamilton believes that patients do best, long-term, with permanent repair as this returns the nose to normal function. Dr. Hamilton’s method of surgical repair is over 99% successful in relieving symptoms, closing the perforation, and stabilizing the nose. Learn more
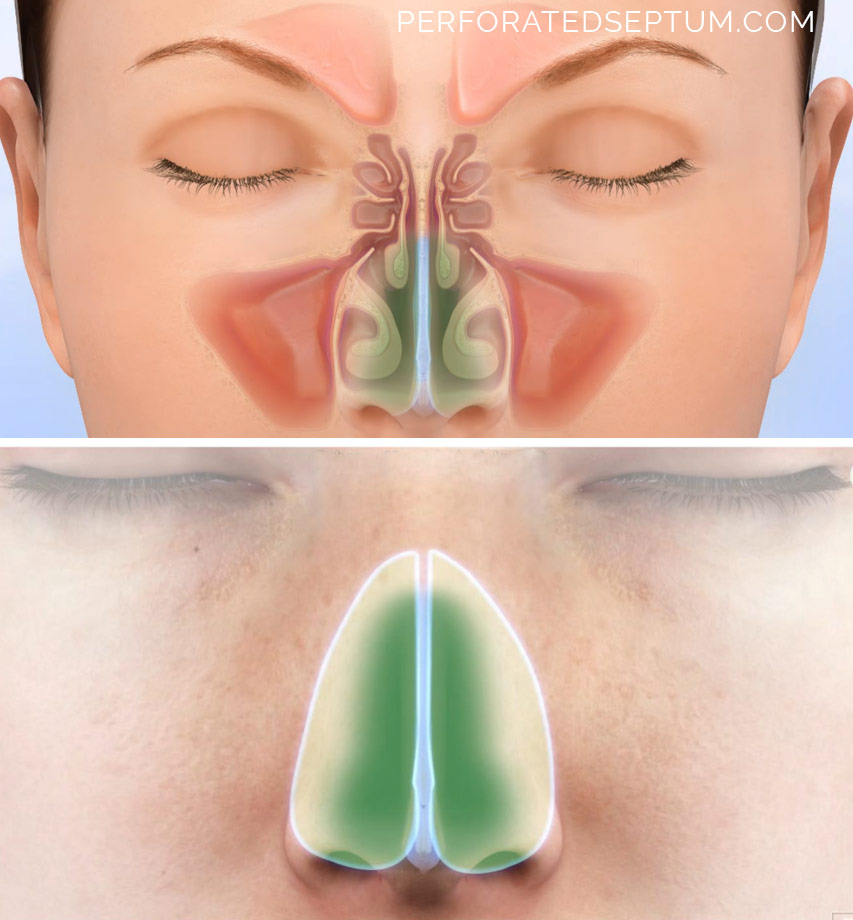
Hamilton’s Surgical Approach
TO PERFORATED SEPTUM SURGERY
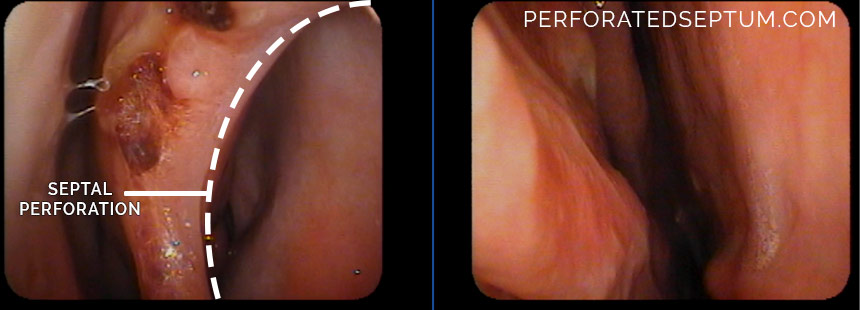
This patient had the Hamilton Method of septal perforation repair, which requires no skin grafts, no cartilage grafts, and leaves the nasal turbinates undisturbed. Preoperative and postoperative exam are performed 4 weeks apart.
Surgical SuccEss Rate OF PERFORATED SEPTUM SURGERY
Treatment options for septal perforation are poor and most institutions and private physicians’ success rates hover around 10-45%. Dr. Jason S. Hamilton, MD has developed a method for surgical repair of septal perforations with a success rate over 99% for small and large septum perforations.
Why is Dr. Hamilton’s success rate so high compared to others?
Dr. Hamilton’s high success rate is rooted in his ability to perform septal perforation surgery via several different techniques he has developed. The challenge surgeons have is that because the operation is difficult to perform they have only mastered one way of performing the surgery. The problem with this is one way doesn’t fit every surgical scenario. Dr. Hamilton developed his technique because the techniques used by other surgeons had many pitfalls and did not rely on good surgical principles.
Choosing a Surgeon? What is the most important question to ask?
Most surgeons do not perform septal perforation repair. Those that perform septal perforation surgery do it infrequently and have one technique they use for all cases. Unfortunately one size does not fit all cases. Here is the most important question you must ask when choosing a surgeon:
During my surgery, Doctor, if you realize that with your technique you are not going to be able to completely close the perforation (on both sides) then what are you going to do?
You will likely hear:
1. – We will leave it open and it should be all right or
2. We will come back and fix it again with a second surgery
Dr. Hamilton’s Method: Dr. Hamilton found these answers unacceptable for his patients, which prompted the development of his unique methodology
SURGERY FACTS:
- Septum is repaired to its natural state, full mucosa both side of the nose- NO SKIN GRAFTS
- Recovery time is equivalent to other septal perforation techniques-NO DIFFERENCE IN RECOVERY TIME
- Dr. Hamilton has mastery several techniques for closure of various sized perforation
- Dr. Hamilton performs revision surgery for failed repairs attempted by other surgeon
- Has successfully treated patient for all over the world
- No two patients have the same procedure. The surgery is tailored to the individual patient based on size, location, cause of injury, presence of nasal deformity, etc.
Recommendation: Dr. Hamilton recommends surgical intervention to permanently repair all septal perforations. Dr. Hamilton’s success rate is currently over 99%. Please take time to read through the various case presentations successfully treated. Please contact us today to schedule a consultation to discuss your options for treatment and repair of your septal perforation.
Schedule your septal perforation consultation with Dr. Hamilton today.
